View our new Radical Guide to Collaboration.
WORKING TOGETHER FOR A BETTER WORLD
The Radical Guide to Collaboration is based on the hard learnings and personal stories of a team of six people across three very different organisations in Australia who came together to find systems-level solutions for community health challenges (The Culture Well Project, detailed below). We called this guide radical because unlike most guides on collaboration we’re openly sharing what went wrong in our project, what our hard lessons were, and how others can avoid them. We’ve tried to get beyond motherhood statements and surface sentiments to talk about the sticky, challenging reality of working closely with other human beings who may have different backgrounds, languages, needs, pressures and agendas.
About Culture Well
Culture Well is a unique place-based approach to addressing chronic disease. From the use of an innovative research methodology, framework and process (Luke Cravens Systems Mapping, Effects and Wellbeing Wheels), we’re able to understand and analyse the unique social determinants and impacts on health and wellbeing with the community. Through collaboration and co design – putting the person’s life and health at the centre, we can engage communities and prioritise their needs and inform necessary interventions to influence systems change.
Tackling asthma in vulnerable communities
 In Australia, 12 million people have chronic conditions like heart disease, stroke, cancer, diabetes, asthma and mental illness. Many have more than one. They are long-term conditions that have a huge impact on people’s lives, our health system and the economy. They are often described as ‘lifestyle diseases’ that are preventable through healthy living. However, this oversimplified view fails to acknowledge that much of the cause of chronic disease is linked to environmental, economic and social factors, and strongly influenced by social disadvantage: 85% of early deaths from chronic diseases occur in disadvantaged communities.
In Australia, 12 million people have chronic conditions like heart disease, stroke, cancer, diabetes, asthma and mental illness. Many have more than one. They are long-term conditions that have a huge impact on people’s lives, our health system and the economy. They are often described as ‘lifestyle diseases’ that are preventable through healthy living. However, this oversimplified view fails to acknowledge that much of the cause of chronic disease is linked to environmental, economic and social factors, and strongly influenced by social disadvantage: 85% of early deaths from chronic diseases occur in disadvantaged communities.

Research shows that lifestyle factors make up only 30%, while socioeconomic factors like income, housing, our language skills create 40% of our health1. Healthcare only contributes 10% towards our health outcomes, but money continues to be directed to healthcare and medical research, because social disadvantage is much harder to change and to measure.
Our Why…
In public health, we tend to focus on the specific diseases a person has and treat these as separate conditions, but the lived experience of most people with chronic disease is more complex than this. Many people have multiple conditions that intersect with other areas of their lives such as social issues, economic constraints, culture, family demands and access to suitable healthcare. These factors influence the development of chronic diseases, their effective management and the impact that chronic disease has on a person’s life. Turning the tide on chronic disease will require complex prevention strategies that take a whole-of—community health and wellbeing approach. These strategies require long-term funding, and many organisations working together in genuine collaboration.
What are culture well project aims
- Increase collaboration between local health and social organisations and community members to mutually address community identified health and wellbeing issues.
- Create a practical model that can be adapted for different communities that supports organisations to implement a collaborative, social determinants approach to tackling chronic disease.
- Advocate for the importance of systemic, community-centric approaches in public health.

RESEARCH METHODOLOGY AND FRAMEWORK
Systems mapping allows us to explore the complex nature of health and how health interconnects with other areas of life.
This methodology is particularly useful in understanding the user experience of a system: in this case their health, because it is based on two facts:
- the specific determinants or causes of good health and/or ill health are diverse and based on individual circumstances and context
- the connections between the determinants will differ for each individual.

Our Research Findings
- Solutions to chronic disease management including asthma need to focus on the social components and that means focussing on people, and their lives.
- People with chronic diseases including asthma are the experts in how to address the social aspects of their condition in their lives and should lead solutions.
- In treating chronic disease, it is not the specific condition that is important but the context of the life of the person with the disease and where they live.
- New ways are needed because the incidence of chronic disease is rising with the current approaches.
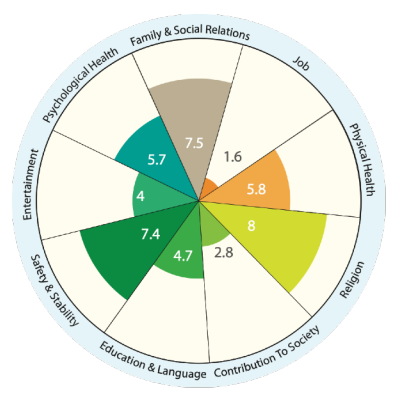
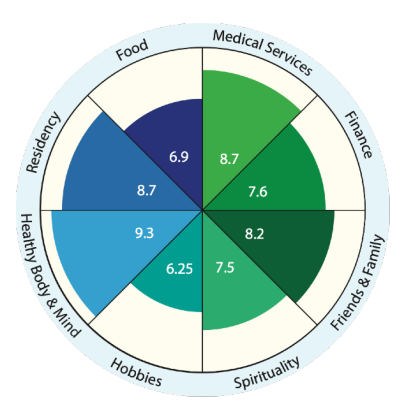
| Arabic Wellbeing Wheel | Vietnamese Wellbeing Wheel | Samoan Wellbeing Wheel |
 |
 |
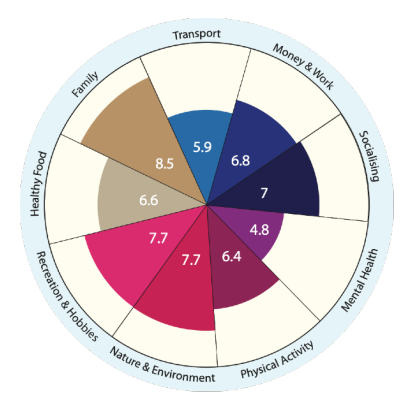 |
Reading the Wheels: The different spokes represent the most important areas of life that contribute to health and wellbeing for this community. The numbers represent how well this area of life is being fulfilled for the group (10 is the highest).
Read our Culture Well Arabic Community Data Report
What are we doing?
Asthma Australia is leading this project and working with Partners in order to change the thinking about how asthma and chronic diseases are managed.
- ✔ Identify communities that are ready for intervention
- ✔ Partner with key, local stakeholders to help connect with and understand local community factors
- ✔ Hold focus groups and do systems mapping with community members to understand their definition of wellness, and the underlying complex social drivers in health and wellbeing in their community
- ✔ Hold focus groups with the service provider community to explore and discuss mapping data, share insights into the underlying drivers of poor health outcomes and seek their perspectives
- Facilitate a collaborative co-design workshop with representatives from both the community and service providers to explore potential intervention points to address the identified drivers of poor health
- Facilitate the development of a collective impact project and roll out with the community
- Mentor the community for 6 -12 months to develop leadership and ownership of the program to implement the co-developed solutions
- Repeat in the next community.
Our Partners
For more information on the program, contact [email protected].
References: 1D. R. Williams, M. V. Costa, A. O. Odunlami& S. A. Mohammed., ‘Moving Upstream: How Interventions That Address the Social Determinants of Health Can Improve Healthand Reduce Disparities’, Journal of Public Health Management Practice, 14/6 (2008), 8. 2M. Rosato et al., ‘Community participation: lessons for maternal, newborn, and childhealth’, The Lancet, 372 (2008), 969 3The Royal Children’s Hospital, Place-based Initiatives Transforming Communities (2012).





 1800 278 462
1800 278 462





